患者需要了解的关于Aduhelm (aducanumab) 的一切信息|新阿尔茨海默病医学
最后更新。2022年3月15日

即使新药在您的国家未获批准,您也可以合法获取。
如何学习文章由Jan de Witt博士审阅
2021年6月7日,美国食品和药物管理局批准了阿杜卡努单抗(以商品名"Aduhelm"生产)用于治疗阿尔茨海默病,提高了世界各地数百万阿尔茨海默病患者及其家人的希望,同时专家们对这一决定表示担忧。
Aduhelm 是18年来美国食品和药物管理局批准的第一种治疗阿尔茨海默病的药物。这种药物声称,根据公布的结果,它能够减缓阿尔茨海默病本身的进展,而不是缓解其症状。
美国食品和药物管理局批准该药品的决定充满了争议。尽管如此,Aduhelm 的制造商Biogen公司预计到2021年6月底开始向美国的900多个医疗中心运送Aduhelm 。
Aduhelm 目前可供美国以外的合适病人以同情心使用或指定病人的方式使用。通过跳转到 "在美国以外获取Aduhelm "部分了解更多信息。
阿尔茨海默病:21世纪的主要社会、医疗和经济危机之一
阿尔茨海默氏病是一种退行性脑部疾病,如今影响到全世界4000多万人,是导致痴呆症的最常见原因。多年来,人们认为阿尔茨海默病是衰老的一个正常部分,但现在已被认为是一种具有严重医疗保健、经济和社会影响的疾病。
研究人员尚未完全了解阿尔茨海默病的原因,但据信它是由多种因素造成的,如:。
- 衰老。阿尔茨海默氏症最常在65岁以后被诊断出来(晚发性阿尔茨海默氏症)。大约三分之一的85岁及以上的人患有阿尔茨海默氏病。大脑中与衰老有关的变化可能会导致该病的发生。
- 家族史。有一个患有阿尔茨海默氏症的一级家族成员会增加一个人患这种疾病的风险。科学家们认为,遗传易感性可导致早发性阿尔茨海默氏症,这种疾病发生在30多岁到60多岁的人身上。只有10%的阿尔茨海默氏症患者有早发的疾病形式。
- 其他因素。科学家们已经发现认知能力下降与心脏病以及糖尿病和肥胖症之间的联系。最有力的证据是将大脑健康与心脏健康联系起来。头部受伤也与阿尔茨海默氏症的风险增加有关,因为它们可以引发淀粉样斑块的形成。患有唐氏综合症的人,其中一个额外的染色体决定了与阿尔茨海默氏症有关的一种淀粉样蛋白的基因编码,其风险也会增加。
大多数阿尔茨海默病患者被诊断为轻度阶段,此时症状变得更加明显,疾病已经造成了一些脑损伤,尽管有些症状甚至在诊断前十年就开始出现。早期症状可能被患者忽视(通常是由于羞愧),或者根本没有被医生或家庭成员注意到。患者在诊断后的平均预期寿命为3-11年。
"久而久之,妈妈忘记了我是谁"
阿尔茨海默氏病有三个不同阶段。
- 轻度。在最初阶段,患者的记忆力下降,如忘记重要的日期和事件,经常重复问题,需要更长的时间来完成日常工作,在财务上经常出现问题,经常放错物品,以及焦虑。要了解更多关于随着年龄增长,记忆力下降的程度是正常的,请看美国国立卫生研究院(NIH)的国家老龄化研究所的信息图)。
- 中度。随着病情的发展,患者的记忆力减退和混乱程度增加,交流和阅读困难,穿衣等日常工作困难,认不出家人和朋友,出现偏执、幻觉和游荡。
- 严重的。严重的阿尔茨海默氏症患者会出现无法沟通、体重下降、吞咽困难和失去对肠道或膀胱的控制。在这个阶段,患者大部分时间都躺在床上,完全依赖他人的照顾。
阿尔茨海默病患者的困难是可怕的,因为这种疾病影响到他们日常生活的各个方面。下面你可以读到一些病人或病人的朋友和家人的故事。
桑迪,一位前牙医和哈佛大学的助理教授,向CNN记者谈到他意识到他的健忘症已经发展到了更严重的程度:"'我在看一个牙科病例档案,看了一个半小时,'他回忆说。'我在读它,它在我的大脑里。然后我就会合上文件,而实际上不记得关于这个案子的任何事情。"不久之后,他被诊断出患有阿尔茨海默病。
弗雷德-沃克(Fred Walker)的妻子被诊断出患有阿尔茨海默病,他向英国阿尔茨海默病研究中心谈到了他的妻子。"'使用电话变得超出了她的能力。她无法掌握所有的按钮。炊具太复杂了,难以理解,而且她总是有不关煤气的危险。她发现泡茶太麻烦了,而且会对需要多少茶、牛奶和水感到困惑"。
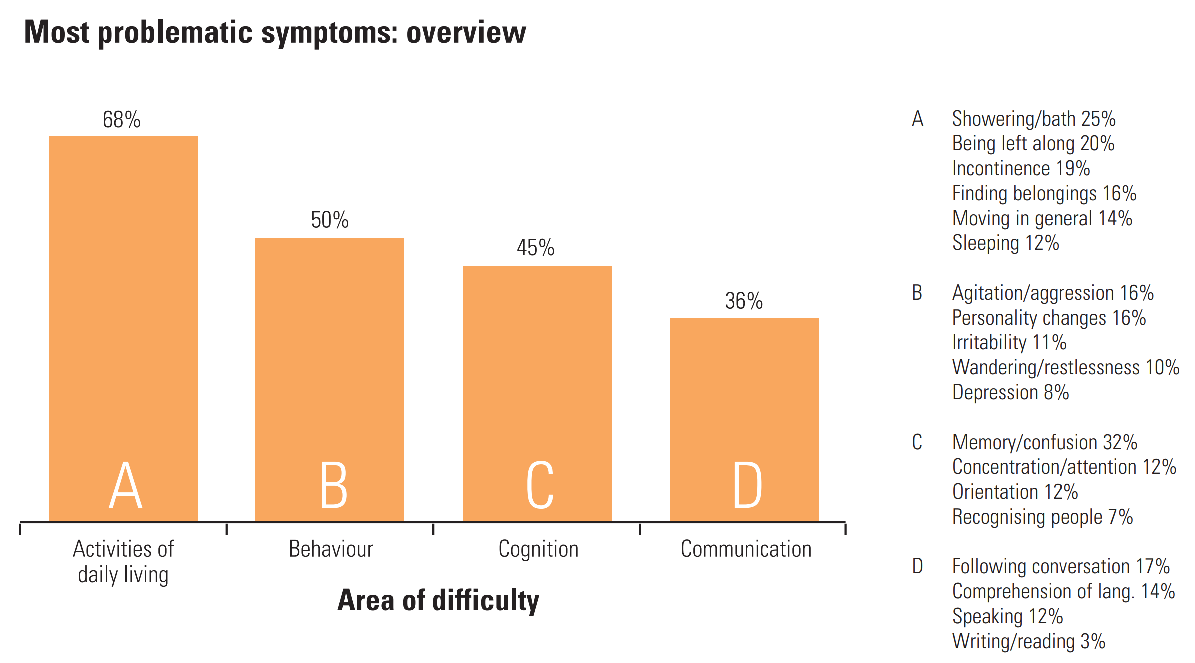
阿尔茨海默病在达到后期阶段并发展为痴呆症时,由劳瑞为阿尔茨海默病协会描述。
"[...]我们开始了新的旅程。这涉及到24小时的护理,每天的药物巡视,以及妈妈完全迷失在她自己的头脑中的迷雾。直到那一刻,我们才意识到,看着自己的亲人患上这种残酷、阴险的疾病,实际上是一场完全恐怖的表演。她开始产生幻觉。
everyone.org 创始人斯亚克-温克(Sjaak Vink)证实并认可这些描述。他的母亲在 2015 年被诊断出患有阿尔茨海默症。
对病人和他们的亲人来说,这是一条艰难的道路--而且这种疾病并不局限于只影响他们的个人生活和他们亲人的生活。
照料者、预算和政策制定者的压力
阿尔茨海默氏症患者随着病情的恶化,需要越来越多的护理,如家庭护理、夜间护理、家政服务或护理;最终,患者可能需要住在辅助生活设施或养老院。这种疾病对病人、他们的家庭成员(他们往往致力于照顾病人)以及个人和国家的预算都造成了沉重的负担。
家庭照顾者在照顾患有阿尔茨海默病的亲人时面临着艰难的使命。一项调查发现,英国95%的家庭照顾者说这影响了他们的身体或精神健康,69%的人报告说经常感到疲惫,64%的人感到焦虑,49%的人感到抑郁。
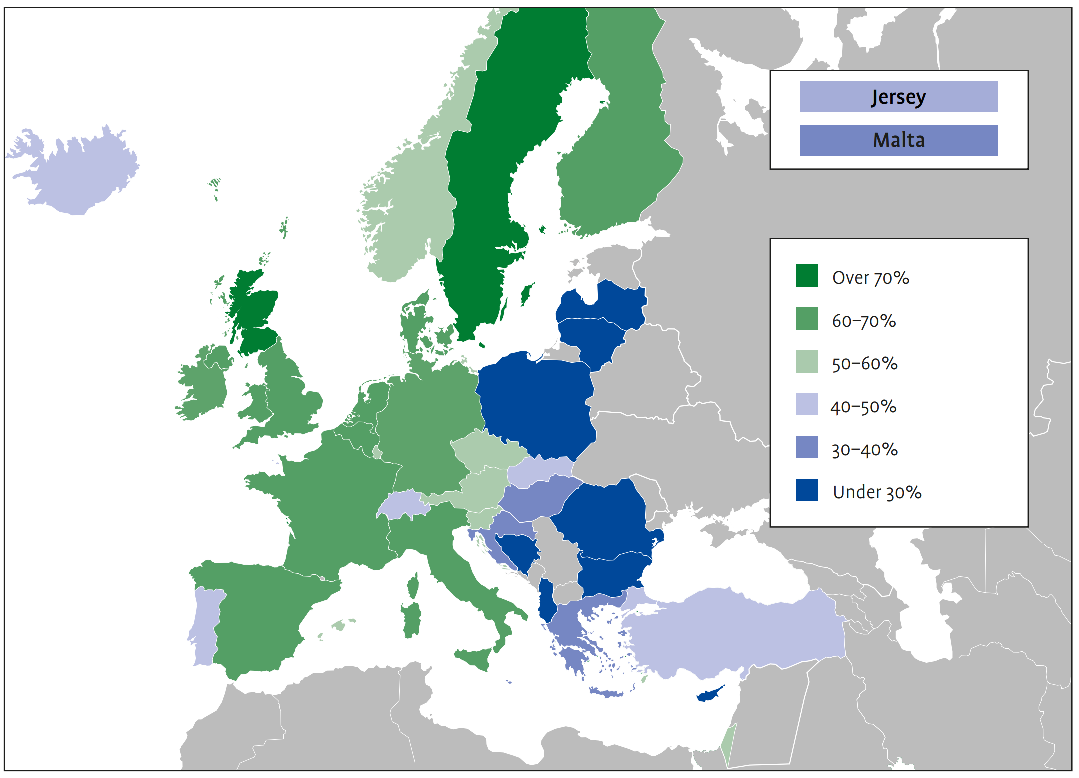
在欧洲,阿尔茨海默病和其他形式的痴呆症影响着大约1000万人,预计到2030年这一数字将增加到1400万人。据估计,到2030年,欧洲痴呆症的经济成本将增加到2500亿欧元以上,其中50%以上是由于非正式的护理费用。获得护理和治疗的机会不平等,特别是在东欧,缺乏针对阿尔茨海默氏症患者及其护理者的可用支持系统和社会方案。
在美国,阿尔茨海默氏病最近进入了十大死因名单,并且是十大死因中唯一没有已知治愈方法的疾病。它影响着美国的600万人,预计到2050年这个数字将增加到1200万人。到2021年底,照顾阿尔茨海默氏症和其他痴呆症患者的全国总成本可能达到3550亿美元,预计到2050年将达到1.1万亿美元。
这笔资金,尽管看起来是个天文数字,但对于为病人提供足够的支持和尽可能的有尊严的生活是必要的。
由于需要全天候的护理,特别是在后期,如果护理不到位,阿尔茨海默氏症患者就会受到特别大的影响,许多国家或社区都是如此。仅在英国,每年就有数以万计的痴呆症患者因感染、跌倒和脱水而被送进急诊室,这些都是由于护理不足造成的。这进一步加重了国家医疗预算的压力。
在COVID-19大流行期间,阿尔茨海默氏症患者受到严重打击,由于年龄、其他长期健康状况和阿尔茨海默氏症本身的挑战(如记忆问题和混乱,使患者难以遵循防止COVID-19感染的准则),死亡人数很高。
护理院的阿尔茨海默氏症患者在其他方面也感受到了破坏性后果。由于照顾不周,为了保证他们免受COVID-19的伤害,他们被迫与亲人分离,随之而来的孤独和寂寞使他们的精神和身体健康进一步恶化。
需要对该疾病进行有效的治疗,以阻止健康和经济危机达到严重的程度。
阿尔茨海默病研究中的亮点
1910年,德国医生埃米尔-克莱佩林(Emil Kraepelin)以医生阿洛伊斯-阿尔茨海默(Alois Alzheimer)的名字将该病症命名为 "阿尔茨海默病",他在一名记忆力极度衰退且心理变化不断恶化的病人身上发现了先兆性痴呆的病理特征。对阿尔茨海默病的治疗研究在20世纪80年代末才在美国开始,但面临着批评,因为医生仍然认为阿尔茨海默病是衰老的必然结果。
1978年在美国,国家老龄化研究所(NIA)和阿尔茨海默氏症协会与辉瑞公司合作,开始了第一个治疗阿尔茨海默氏症症状药物的临床试验。该药于1993年被批准。根据公布的结果,康宁(他克宁)改善了一些病人的认知能力,但并没有阻止疾病的恶化。
在接下来的十年里,又有六种药物获得批准,都是用于治疗阿尔茨海默病的认知症状。
- Aricept(多奈哌齐):用于治疗与记忆和思维有关的症状。
- Razadyne(加兰他敏):用于治疗与记忆和思维有关的症状
- Exelon(利凡斯提明):用于治疗与记忆和思维有关的症状。
- Namenda (memantine): 改善记忆、注意力、理智和语言。
- Namzaric(美金刚+多奈哌齐):上述的组合。
- Belsomra(Suvorexant):用于治疗阿尔茨海默氏症患者的失眠症
最后一种被批准用于治疗阿尔茨海默病的药物是在2003年被批准的。几十年来,阿尔茨海默氏病被认为是衰老的自然结果。很少有资源被用于寻找治疗方法,因为人们对它是否是一种真正的疾病存在争议。然而,在过去的20年里,研究人员已经将大量的资源用于研究该疾病和开发治疗方法。
阿尔茨海默氏症缺乏治疗方法并不是因为制药公司方面的忽视--整个行业已经在研究方面投入了数十亿美元。仅礼来公司就在三十年间花费了42亿美元试图开发一种成功的药物,而美国国立卫生研究院(NIH)每年在研究和开发治疗方法方面的花费超过5亿美元。
自2013年以来,美国国会已将NIH用于阿尔茨海默氏症研究资金和相关痴呆症的年度预算增加了两倍,在2019年达到31亿美元。
国家和私人资金导致2019年进行了2173项临床试验,以测试各种理论。所测试的顶级理论。
- 19%的试验集中在神经递质假说上
- 17.0%的试验测试了线粒体级联假说和其他相关假说
- 12.7%测试了陶氏传播假说
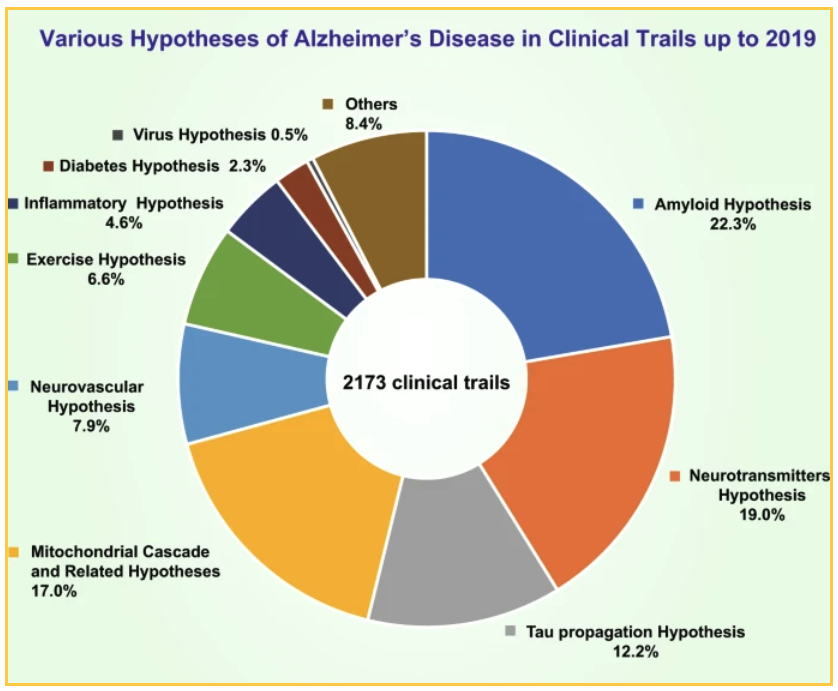
针对淀粉样蛋白的22.3%的试验侧重于减少斑块的不同方式。
- 免疫系统产生的针对β-淀粉样蛋白的抗体。"活性疫苗",当注射到体内时,触发免疫系统产生抗体来破坏β-淀粉样蛋白并降低大脑中的β-淀粉样蛋白水平。
- 实验室生产的β-淀粉样蛋白的抗体。"被动疫苗",它被认为比试图在体内诱导产生抗体更有效和更安全。
- 减少β-淀粉样蛋白的产生。一些实验性治疗改变了某些蛋白质的行为,可以防止或减少β-淀粉样蛋白的产生。
- 防止β-淀粉样蛋白的聚集。科学家们正在研究防止β-淀粉样蛋白和脑细胞之间最初的相互作用而导致脑细胞死亡的药物。
- 增加β-淀粉样蛋白的清除。调动免疫系统来攻击β-淀粉样蛋白或施用具有抗淀粉样蛋白作用的天然制剂等技术。
- 具有抗淀粉样蛋白作用的天然制剂。从人类献血者那里获得的静脉免疫球蛋白(IVIg)含有天然抗体,可以降低β-淀粉样蛋白水平。
什么是Aduhelm (aducanumab-avwa)?
Aduhelm (aducanumab)是一种抗淀粉样蛋白抗体,适用于治疗阿尔茨海默病。它旨在清除阿尔茨海默病患者在脑细胞之间形成的数量异常的β-淀粉样斑块,这些斑块导致受影响的脑细胞死亡。β-淀粉样蛋白于1984年被发现,并很快被认为是脑细胞损伤的主要触发因素,而在1986年,tau蛋白被发现,它是缠结的关键成分和脑细胞恶化的第二个触发因素。
Aduhelm 是由位于美国马萨诸塞州的跨国生物技术公司Biogen, Inc.开发的。Aduhelm 是以每月注射方式给药。
Aduhelm ,有着悠久的历史。
瑞士生物技术公司Neurimmune Therapeutics AG与苏黎世大学合作,在健康老人和缓慢进展的痴呆症患者中发现了保护性的抗淀粉样蛋白抗体,并导致了阿杜单抗的发现,即Aduhelm 中的活性成分。在轻度阿尔茨海默病患者中,每月静脉注射阿杜卡努单抗一年,可以减少淀粉样斑块,从而减缓认知能力的下降。
Neurimmune于2007年将治疗阿尔茨海默病的阿杜卡努单抗授权给百健公司,并与百健公司合作开发该药。
Aduhelm 是如何工作的?
阿尔茨海默病似乎是两种蛋白质--β-淀粉样蛋白和tau--在大脑中异常累积的结果。β-淀粉样蛋白是一种正常存在于大脑中的蛋白质,在阿尔茨海默病中,它在脑细胞之间结成淀粉样斑块--淀粉样蛋白理论认为这些斑块损害并最终杀死脑细胞。淀粉样斑块似乎在疾病的早期发展,而tau缠结往往在疾病的后期出现。为寻找阿尔茨海默病的治疗方法而进行的大部分研究都集中在去除淀粉样斑块上。
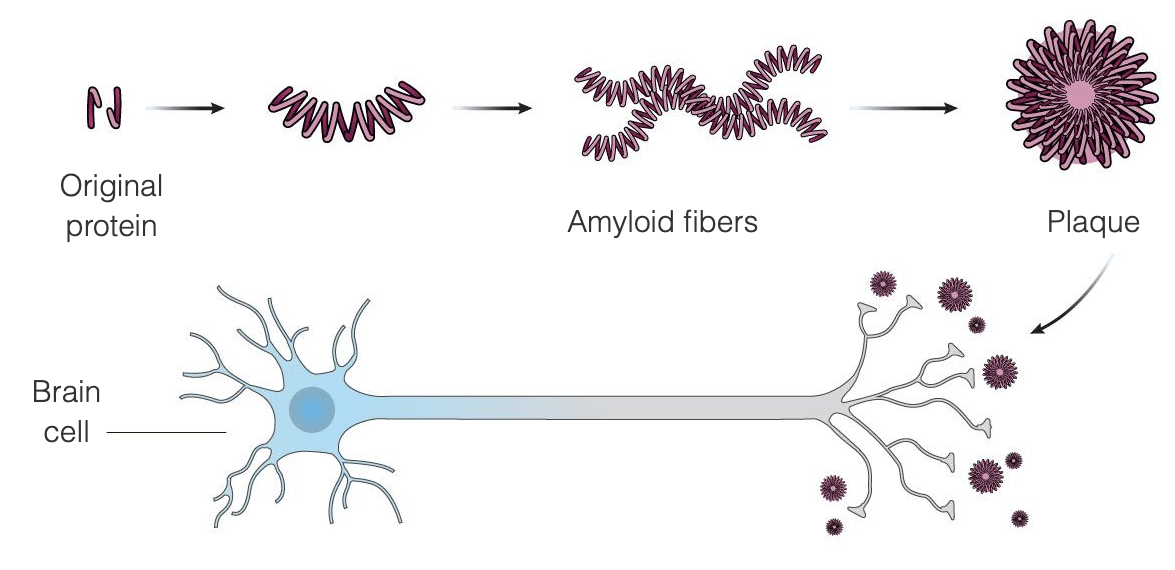
Aduhelm ,旨在通过与淀粉样斑块结合,在疾病的早期阶段治疗阿尔茨海默病,从而触发免疫系统摧毁斑块,将其视为外来入侵者。其目的是,一旦斑块被清除,脑细胞将停止死亡,认知功能将停止恶化。Aduhelm ,利用这一机制,目的是减缓疾病的进展,特别是解决阿尔茨海默病早期阶段的患者。Aduhelm ,不能逆转已经造成的损害。
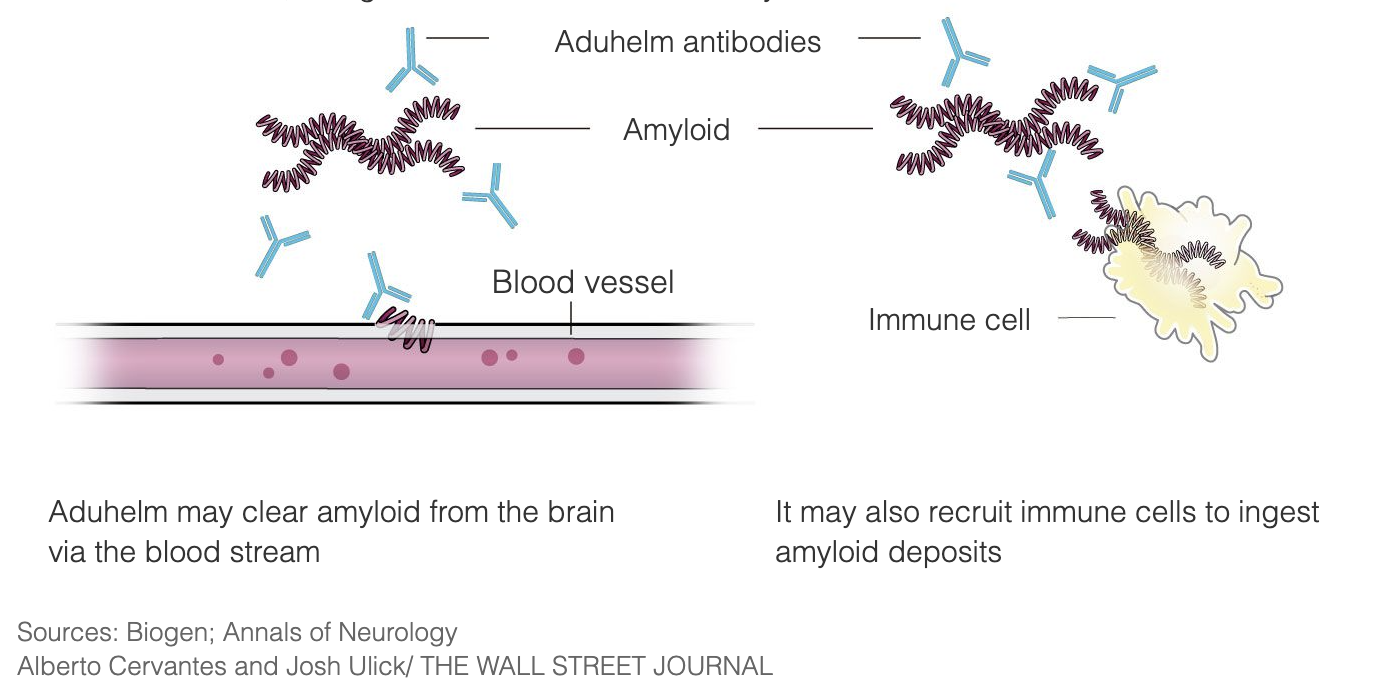
30年来,淀粉样斑块一直是阿尔茨海默病研究和药物开发的目标,而Aduhelm ,是多年来研究的此类治疗方法之一。
"圣爱弥儿教堂"
科学家们尚未就阿尔茨海默氏病的原因达成一致,但他们有某些理论。其中一个被称为 "淀粉样蛋白假说",Aduhelm 是在假设这一理论是正确的基础上开发的。
淀粉样蛋白假说指出,在脑细胞之间形成的淀粉样蛋白斑块导致细胞死亡,从而导致认知能力下降。这是一个长期存在的理论,但从未被普遍接受--迄今为止,针对淀粉样斑块的临床试验的失败,使其批评者更加大胆。一些人称这一理论的支持者为 "神圣的淀粉样蛋白教会",因为他们不愿意甚至拒绝接受其他理论。
甚至连β-淀粉样蛋白在大脑中的正常功能也受到了研究人员的争议,因为他们并不认同它在人体中自然发挥的作用,或者它是否是阿尔茨海默病的严格标志。
对淀粉样蛋白假说的一个常见的反驳是,在许多认知能力正常的老人的大脑中发现了斑块。有趣的是,一些对90岁以上具有非凡记忆的老人进行的尸检发现,他们的大脑中有不同程度的淀粉样斑块--其中一些人的密度很高,类似于最严重的阿尔茨海默氏症,而且他们的神经元也比死于阿尔茨海默氏症的人多很多。
一些研究人员认为,β-淀粉样蛋白实际上可能具有保护作用。
德克萨斯大学圣安东尼奥分校的神经生物学家乔治-佩里认为,"β-淀粉样蛋白和tau的积累实际上是对细胞中与年龄有关的代谢压力的一种保护性反应,"并且特别有助于减少大脑中的氧化压力(氧化压力随着年龄增长而增加,从而损害细胞)。
一些研究已经调查了阿尔茨海默病的其他潜在原因。其中一项研究是由纽约西奈山伊坎医学院的研究人员领导的,他们发现在阿尔茨海默病患者的大脑中发现了两种叫做HHV(疱疹病毒家族的一部分)的病毒株,数量较大。虽然不确定这两种病毒是否会导致这种疾病(更可能的原因是病毒加上某种叫做APOE的基因变体的组合),但数据表明,感染会增加患阿尔茨海默氏症的风险。而接受抗病毒药物治疗的人患阿尔茨海默氏症的可能性会降低10倍。
然而,支持淀粉样蛋白理论的是一些遗传学发现,它们将与淀粉样蛋白有关的基因问题与早发性阿尔茨海默病的发展(在30至65岁的人群中)联系起来。唐氏综合症被认为是一个风险因素,因为研究人员发现,唐氏综合症患者有一个额外的染色体拷贝,该染色体包含编码与早发性阿尔茨海默病有关的淀粉样蛋白的基因。
其他基因异常可能导致产生更容易形成斑块的β-淀粉样蛋白的较长变体,或增加β-淀粉样蛋白的产生,并导致有点罕见的早发阿尔茨海默病。一个家族的多个成员可能携带这些基因突变,增加个人患早发性阿尔茨海默病的风险。
淀粉样蛋白理论的支持者表示,早期涉及针对淀粉样蛋白斑块的药物试验只是存在缺陷。例如,一项关于semagacestat的研究,一种抑制β-淀粉样蛋白产生的抑制剂,使研究参与者的认知能力恶化;研究人员还观察到参与者中皮肤癌的增加。这可能是由于semagacestat也抑制了其他蛋白质的产生,而不仅仅是β-淀粉样蛋白,其中一些蛋白质在人体中具有重要的功能。
对于这些针对淀粉样蛋白的试验的失败,最得到支持的解释是,这些药物是正确的药物,但在阿尔茨海默病进展的错误点上用药--在形成淀粉样蛋白斑块的过程中用药太晚,而这个过程在症状出现前几十年就开始了。
肯塔基大学的神经科学家迈克尔-墨菲指出,"'我们可能已经有了一种可以治疗阿尔茨海默病的药物,如果我们把它给50多岁的人服用。
关于阿尔茨海默氏症的病因有很大的争论,专家们的意见还不一致--但患者和研究人员在Aduhelm的一项3期临床试验中获得了阿杜卡努单抗的结果,这给他们带来了新风。
Aduhelm 在临床试验中
临床试验分四个阶段进行。
- 第0阶段:在少于15名参与者身上进行极少量的药物测试,以确保其无害,并确保试验能够继续进行。
- 第一阶段:在20至80名没有潜在健康状况的参与者身上测试该药品,以确保没有严重的副作用。根据美国食品和药物管理局的数据,大约70%的药品进入第二阶段。
- 第二阶段:在几个月或几年的时间里,在几百名患有该药的参与者身上测试该药,以收集关于其有效性和副作用的信息。大约33%的药品进入第三阶段。
- 第三阶段:该药在多达3000名患有该药所要治疗的病症的参与者身上进行测试,并可持续数年。该药品必须被证明是安全和有效的。25-30%的药品进入第四阶段。
- 第四阶段:这一阶段涉及数千名参与者,持续多年,在美国食品和药物管理局批准该药品后进行。其目的是为了收集更多关于其长期安全性和有效性的信息。
Aduhelm 在第1阶段
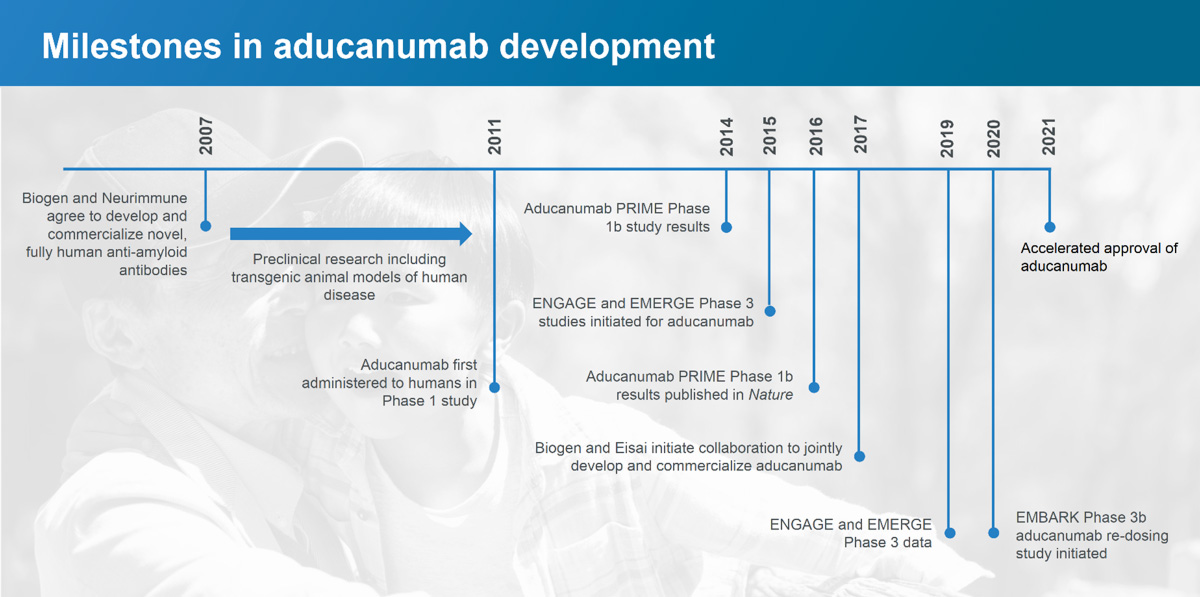
百健公司进行了几项调查阿杜卡努单抗的临床试验,从2011年的三项1期试验开始,在美国和日本的健康志愿者和阿尔茨海默病患者中测试阿杜卡努单抗,使用不同剂量的阿杜卡努单抗和安慰剂。一些患者的入组时间超过3年。
2016年,百健公司公布了他们的1期临床试验结果,研究人员对患有轻度阿尔茨海默病的试验参与者每月静脉注射阿杜卡努单抗一年。接受阿杜卡努单抗治疗的参与者大脑中的β-淀粉样蛋白水平降低了,而且根据官方的临床痴呆评级,认知能力下降的速度减缓了。在接受aducanumab输液的参与者中,百健公司的研究人员还记录了ARIA(淀粉样蛋白相关的影像学异常,如脑水肿或脑出血)等副作用的减少。百健公司发现这些结果足以令人鼓舞,从而进入第二阶段。
Aduhelm 在第2阶段
百健公司在2018年底开始了2期试验,除了检查早期和有症状的阿尔茨海默病参与者的淀粉样斑块减少和认知能力下降放缓外,还评估了继续服用阿杜卡努单的安全性。
Aducanumab未能实现其主要目标,即在12个月时显示出较慢的认知能力下降,但在重新分析了18个月的试验数据后,在五个剂量中的一个--最高剂量的Aducanumab中观察到了积极效果。最高剂量被证明能减少大脑中的淀粉样斑块,并对认知能力有积极的反应。
与第一阶段一样,在所有参与者中约有10%观察到副作用,如ARIA(淀粉样蛋白相关的成像异常),在接受最高剂量阿杜单抗的参与者中不到15%。
"BAN2401试验的18个月结果令人印象深刻,为淀粉样蛋白假说提供了重要支持,克利夫兰诊所Lou Ruvo脑健康中心创始主任Jeff Cummings在为生物空间公司发表的一份声明中说。
Aduhelm 在第三阶段
在2期试验结果出来后,百健公司进行了两项3期试验,名为Engage和Emerge,在北美、澳大利亚、欧洲和亚洲招募了近3300名患有相对轻度阿尔茨海默病的参与者。Aducanumab以低剂量和高剂量注射到血液中,每月一次,与接受安慰剂的参与者的结果进行比较。
2019年3月,百健公司停止了这两项三期研究,理由是一个独立的数据监测委员会进行了徒劳性分析,认为阿杜单抗似乎没有达到预期效果。
这一决定影响了3300名研究参与者。参加研究的方案涉及频繁和长时间的访问,包括抽血、核磁共振成像、PET扫描,有时还包括脊柱穿刺。在停止这两项研究的七个月后,百健公司宣布,对其他数据的重新分析表明,在高剂量下,该药似乎可以减少认知能力的下降。
百健公司在一份新闻稿中写道,额外的数据由3期Engage研究中的一个子集的结果组成,这些患者接受了高剂量的aducanumab,认知和功能障碍(记忆、定向、语言)明显减少,并对日常生活中的活动(做家务、购物、独立外出旅行)有好处。基于这些结果,百健公司于2019年10月申请了阿杜卡奴单抗的监管批准,并于2021年6月初获得批准。
尽管3期临床试验对该疗法在认知和功能方面的益处没有完全定论,但美国食品和药物管理局认为,这些试验表明,以商品名Aduhelm ,阿杜卡奴单抗可以减少淀粉样斑块,这构成了美国食品和药物管理局加速批准决定的基础。
试验参与者和记者Phil Gutis为Being Patient新闻平台写道:"我通过纵向研究PET扫描得知,我的大脑中不再有任何淀粉样物质。大约两年前,作为宾夕法尼亚州记忆中心的大脑老化队列研究的一部分,这次扫描证实了我越来越多的预感,即阿杜卡奴单抗确实在帮助我。我开始感觉到我正在从持续的精神迷雾中走出来......从消极方面看,我失去的记忆并没有恢复。"
的副作用和禁忌症Aduhelm
根据Biogen公司的用药指南,在考虑Aduhelm ,患者应告知他们的医疗服务提供者所有的医疗条件,包括是否有。
- 正在怀孕或计划怀孕
- 正在进行母乳喂养或计划进行母乳喂养
患者应该告诉他们的医疗保健提供者他们所服用的任何药物,包括处方药和非处方药、维生素和草药补充剂。
根据Biogen公司的用药指南,Aduhelm ,已知的主要副作用是ARIA(淀粉样蛋白相关成像异常),如脑水肿和脑出血。其他的副作用是。
- 严重的过敏反应,如脸部、嘴唇、口腔或舌头的肿胀和荨麻疹
- 头痛
- 腹泻
- 精神错乱/谵妄/精神状态改变/失调
- 瀑布
ARIA是一种常见的副作用,通常不引起任何症状,但可能是严重的。它最常见的是在大脑中出现暂时性肿胀,通常会随着时间的推移而自行消退。同时,从大脑中清除淀粉样蛋白的同时也清除了血管中的淀粉样蛋白,这可能会在大脑中或大脑表面产生小的出血点。
在临床试验中,41%接受阿杜卡努单抗的参与者观察到ARIA,而接受安慰剂的参与者中只有10%。
虽然大多数脑部区域肿胀的人没有症状,但大约30%的人可能有轻微的症状,如:。
- 混乱
- 头痛
- 晕眩
- 视力变化
- 恶心
已退休的神经学家和长期参与Aduhelm 临床试验的丹尼尔-吉布斯(Daniel Gibbs)分享了他的经验,他遇到了一个极其罕见的ARIA副作用。
"首先,我应该说,这是基本正确的教条,[ARIAs]通常是良性的。大多数人不知道他们有这种病。ARIAs]只在核磁共振扫描中被发现,那里会有一些小的肿胀区域或因出血而出现的小的铁沉积区域。如果人们有这方面的症状,通常是温和的。头痛是最常见的症状,偶尔会出现混乱。
但几乎总是这样,即使是有症状的ARIA,如果你停止用药,它们会在几个月内消失。该药物可以再次安全地重新开始使用。至少在药物制造商Biogen所讨论的案例中,很少有灾难性的ARIA或严重的案例,而我的案例就属于这一类。[...]
我开始有越来越多的头疼。我的头痛并不罕见,所以我并没有真正想到什么,但它们变得更加频繁,也许更加严重,但仍然通过非处方[药物]缓解。[...]
然后在2017年圣诞节前的一两个晚上,我出现了我一生中最严重的头痛,就是那种我们作为神经科医生会联想到蛛网膜下腔出血,大量出血进入大脑。我测了血压,血压高得离谱,而且一直很高,所以我以为我是中风了。
我让妻子带我去急诊室,当我到了当地医院时,我真的无法说出连贯的病史。[...]
但在几天之内,我的情况就有了些许改善。我的头疼消失了,但我仍然有阅读困难。在接下来的一个月里,情况变得有点糟糕。那时我的核磁共振扫描显示这是ARIA,我的大脑到处都有肿胀和出血。由于病情加重,人们认为应该对其进行治疗。我接受了五次大剂量的类固醇治疗,这立即缓解了我的头痛和困惑。但我花了大约六个月的时间,大脑中的肿胀才完全消失"。
鉴于这些罕见但严重的潜在副作用,患者的医疗保健提供者将不得不在使用Aduhelm 治疗之前和期间进行磁共振成像(MRI)扫描以检查ARIA。
批准Aduhelm (阿杜卡努单抗)。
2021年6月7日,美国食品和药物管理局批准加速批准Aduhelm (aducanumab)用于治疗阿尔茨海默氏病。
加速批准是一种批准类型,可以在所有结论性证据提交之前,对在临床试验中显示出积极治疗效果的药品进行批准。这只能适用于治疗严重疾病的药物,以满足未得到满足的医疗需求;上一个被批准用于治疗阿尔茨海默病的药物是在18年多以前被批准。
加速批准是有条件的。FDA要求制造商Biogen进行一项新的临床试验,以验证该药的临床效益。 如果试验未能显示出效益,FDA可能会撤销对该药的批准。百健公司必须在2029年之前完成另一项临床试验,以证实阿杜卡努单抗对阿尔茨海默氏症患者的益处;专家认为,第三项临床试验可以在两年内完成,这比等待八年才知道该药是否有效,而患者接受昂贵的治疗并希望得到最好的结果要好。
一场带有金融色彩的医学争论
美国食品和药物管理局批准aducanumab的决定使专家们感到困惑,他们说没有足够的证据表明Aduhelm 是对阿尔茨海默病的有效治疗。他们中的许多人,包括一个独立小组,向美国食品和药物管理局建议,现有的证据使人们对阿杜卡努单抗可以减缓认知能力的下降产生了重大怀疑,并就两项三期研究中只有一项的积极结果是否是美国食品和药物管理局批准的充分依据进行了辩论。
在批准后不久,三位科学家从为FDA提供治疗建议的独立委员会辞职以示抗议,理由是缺乏令人信服的证据。他们还批评美国食品和药物管理局决定批准阿杜卡努单抗用于任何阿尔茨海默氏症患者,尽管该试验是针对早期阿尔茨海默氏症进行的,并接受了减少淀粉样斑块实际上会减缓其认知症状的理论(尽管科学界对其有效性存在误判)。
美国食品和药物管理局在这些条件下批准阿杜卡努单抗的决定可能会产生若干影响。
- 其他针对淀粉样斑块的药物,如礼来公司的多纳尼单抗,获得批准的速度可能比之前预测的要快,这刺激了制药公司对阿尔茨海默病药物的投资兴趣,或继续参与现有的试验。
- 美国食品和药物管理局的决定创造了一种对监管灵活性的看法,这可能会激励其他生物技术公司开发治疗罕见疾病的药物,在一长串临床试验失败后,特别是在阿尔茨海默氏症治疗批准之间的18年里,这种动力已经消退。
- 这种药相当昂贵,每年5.6万美元,这意味着私人健康保险费率可能会增加,因为保险公司将被要求支付它,而且作为医疗保险(美国国家医疗保险)的一部分,它将增加纳税人的负担。有人说,这对医疗保险来说可能是 "毁灭性的",不仅是由于它的基本费用,而且还因为用Aduhelm ,病人需要通过脊髓穿刺来检测淀粉样蛋白进行早期诊断,并通过核磁共振成像(等)进行持续监测,这大大增加了费用,给医疗系统带来压力。
这一批准也被视为百健公司的意外之财,因为他们的股价上涨了50%以上,而日本合作伙伴卫材公司的股价则攀升了56%。分析师预测,考虑到仅在美国就有600万阿尔茨海默病患者,Aduhelm 可能会获得约100亿美元的销售额。这种药物对百健公司的增长非常重要,因为竞争已经损害了他们的药物--治疗多发性硬化症(MS)的Tecfidera ,以及治疗脊髓性肌肉萎缩症(SMA)的Spinraza 。
Spinraza 是Biogen公司产品组合中另一种价格高昂的药物,其上市价格为治疗的第一年75万美元,此后每年37.5万美元。
并非所有人都对美国食品和药物管理局的批准决定持批评态度Aduhelm
由于阿尔茨海默氏症是一种渐进性疾病,患者需要尽早治疗,而不是拖延。美国食品和药物管理局的决定的消息给许多人带来了新的希望,要么是这种治疗方法对他们自己或他们所爱的人有效,要么是它将刺激其他公司采取行动,开发其他阿尔茨海默氏症的治疗。
患者权益团体曾大力推动批准,因为对于这种令人衰弱的疾病,目前只有六种其他治疗方法,而这些治疗方法只能解决几个月的症状。2020年11月,美国食品和药物管理局咨询委员会投票反对批准Aduhelm ,这引发了阿尔茨海默氏症协会的愤怒,然后采取行动,他们随后开展活动,表达他们对该药物潜力的支持,并强调需要希望和进步。
2021年1月,美国食品和药物管理局与患者团体举行了一次听证会,患者、护理人员、临床医生和倡导者都赞成该疗法,他们认为,除其他外,患者不能再等待治疗。
美国食品和药物管理局新药办公室主任彼得-斯坦恩在一次新闻发布会上证实,患者的意见起到了一定的作用。他说,FDA "非常清楚地听到了病人的意见,他们愿意接受一些不确定性,以获得一种可能对预防这种疾病的发展提供有意义的好处的药物,正如我们都知道,这种疾病可能有非常毁灭性的后果"。
美国食品和药物管理局药物评估和研究中心的代理主任Patrizia Cavazzoni在同一新闻发布会上说,"数据支持病人和护理人员有选择地使用这种药物"。
"阿尔茨海默氏症协会首席科学官玛丽亚-卡里略博士说:"美国食品和药物管理局的这一药物批准开创了阿尔茨海默氏症治疗和研究的新时代。"历史已经告诉我们,一个新类别的第一种药物的批准为该领域注入了活力,增加了对新疗法的投资,鼓励了更大的创新"。
Aduhelm 何时能在欧洲获得批准?
阿尔茨海默病作为本世纪的主要医疗、经济和社会危机之一正在迅速崛起--而且很难在早期发现,特别是考虑到欧洲缺乏能够确认诊断的专家。仅在欧洲,截至2018年,就有970万人患有阿尔茨海默病和其他形式的痴呆症;到2030年,患者人数预计将上升到1400万,这就产生了对有效治疗的迫切需求。
Aduhelm ,尚未在美国以外的国家获得批准。百健公司已申请于2020年10月在欧盟进行监管审查,并在2020年底在日本、加拿大、澳大利亚和巴西进行监管审查。
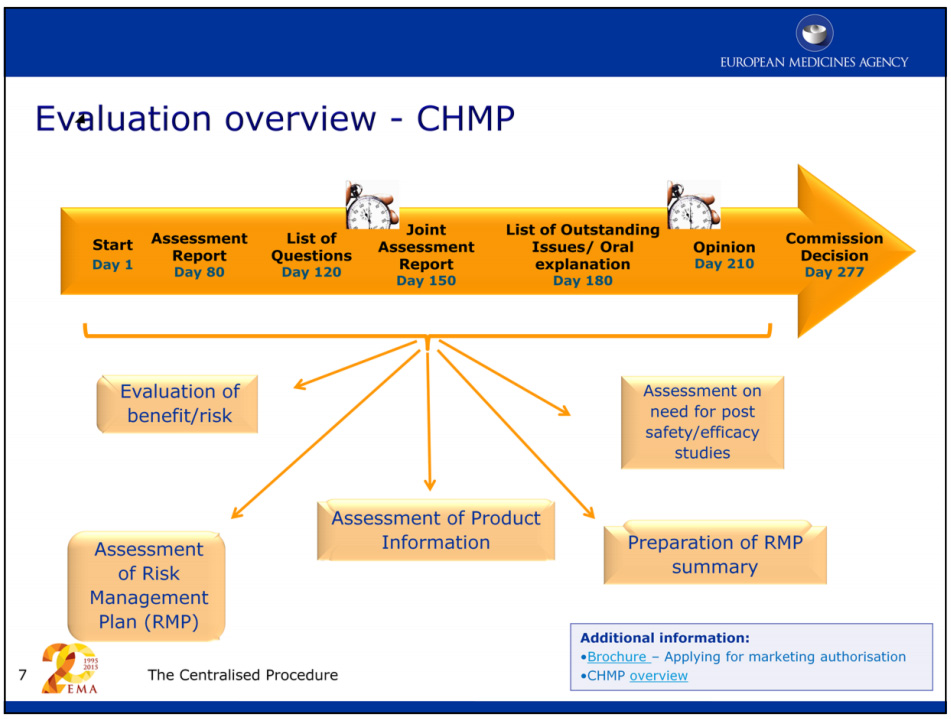
根据欧洲药品管理局(EMA),对新药上市许可申请的评估通常需要一年左右的时间,如果药品开发商获得加速评估,评估时间会更短。
今年3月,百健公司在瑞士投资20亿美元的生产设施获得了瑞士治疗产品机构(Swissmedic)颁发的良好生产规范(GMP)许可证。百健公司计划在2021年底寻求FDA批准在瑞士的工厂生产Aduhelm ,并预计每年向100多万名患者供应该药品。
在美国境外访问Aduhelm
Aduhelm ,目前已获得美国食品和药物管理局的批准,可供美国居民使用--而且有规定允许在目前尚未批准的国家进口药品。
患有危及生命或衰弱疾病的病人有权在其主治医生的帮助下获得、购买和进口药品。
病人和他们的医生可以在同情性使用或指定病人进口条例的基础上进行,这是一般规则的一个法律例外,即通常只有在病人居住的国家获得市场授权/批准(不管我们使用什么措辞)后才能获得药品。这种例外允许病人以合法、道德和安全的方式获得在他们国家尚未批准的药品。
在此阅读更多关于 "命名病人的基础"(EMA)。
everyone.org 我们致力于让患者及其主治医生能够获得全世界范围内的任何药物,以获得最佳治疗。如果您不在美国,我们将 100% 遵守您所在国家的法规。如果您想了解更多详情、获取药品或联系我们的支持团队,请点击此处。
Aduhelm 的费用是多少?
百健公司已经宣布,一个普通病人的维持剂量(10毫克/公斤)的Aduhelm ,每年的费用将是56,000美元。这还不包括患者在治疗前和治疗期间必须做的测试。
百健公司收到了关于该药每年高价的批评。
非营利性的临床和经济审查研究所(ICER)负责分析药品价格,它表示,每个病人每年的公平价格将在2500美元到8300美元之间。ICER在一份声明中说,FDA的批准未能保护患者,百健公司每年可以收取超过500亿美元的费用,"甚至在等待证据来证实患者从治疗中获得实际利益"。
百健公司首席执行官Michel Vounatsos对批评作出了回应,他断言该药物的价格是合理的,因为它将为患者和社会带来较少的阿尔茨海默氏症负担,而且这个价格是 "二十年来没有创新 "的反映。"现在是对治疗进行投资的时候了,"他补充说。
everyone.org ,我们无法影响百健公司制定的价格。我们可以帮助患者按以下价格获得Aduhelm :
- 一瓶170毫克/1.7毫升(100毫克/毫升),价格为1,958.58欧元
- 一瓶300mg/3mL(100mg/mL)的价格为3,046.68欧元
在这里进行查询,以了解更多信息。
即将推出的阿尔茨海默病的治疗方法
2021年5月发表的一项研究显示,目前有126种治疗阿尔茨海默病的临床试验。其中82.5%以改变疾病为目标,10.3%增强认知能力,7.1%专注于缓解神经精神症状。
- 3期试验:28个治疗(包括阿杜单抗)。
- 第2期试验。74项治疗
- 第1阶段试验:24个疗程
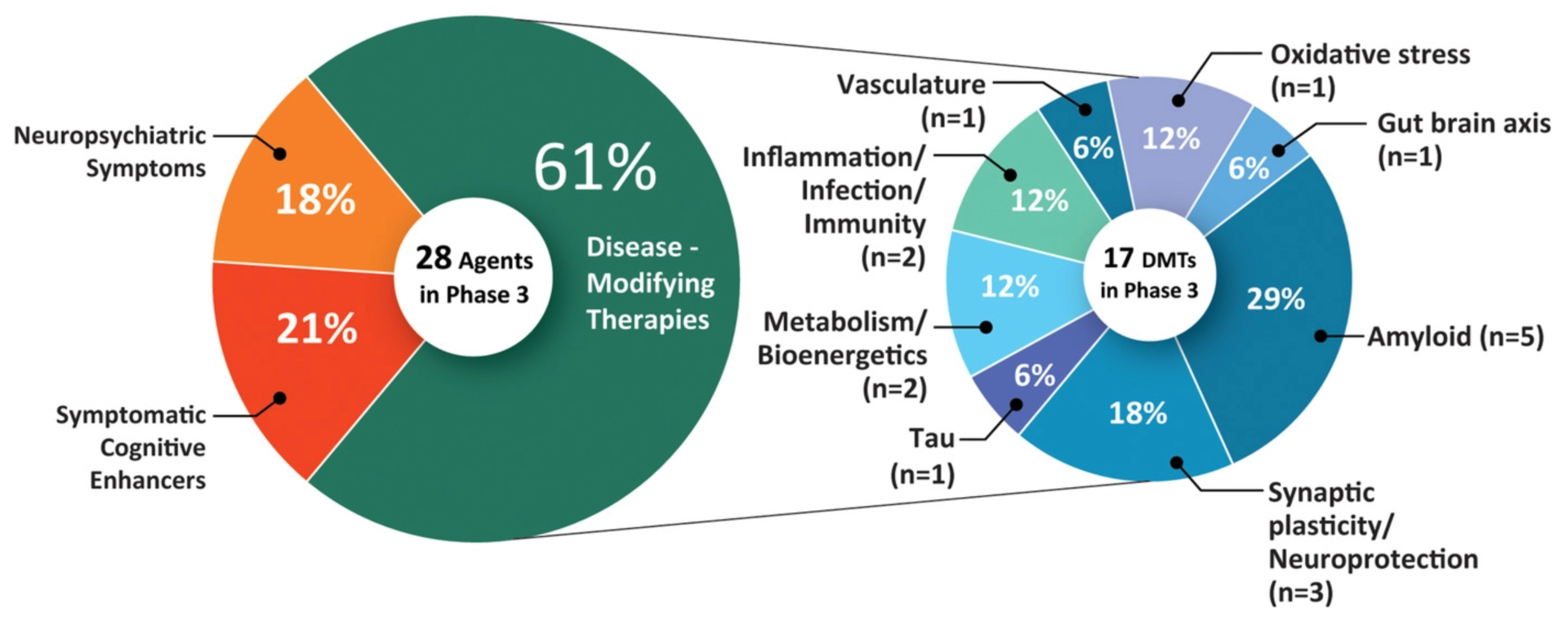
处于第三阶段试验的治疗方法最有可能在未来一年内获得批准。
莱卡尼玛
根据发表的报告,单克隆抗体lecanemab以类似于aducanumab的方式运作(触发免疫系统清除β-淀粉样蛋白斑块),显示出前景,并已进入3期临床试验。
Gantenerumab
Gantenerumab与β-淀粉样蛋白结合,特别是与血液中循环的单个β-淀粉样蛋白相比,与β-淀粉样蛋白的斑块结合。它被认为能够溶解淀粉样蛋白斑块,并通过刺激吞噬作用来清除β-淀粉样蛋白,吞噬作用是指细胞将某种分子纳入自身并将其消化的过程。以前对甘特纳姆单抗的临床研究显示,它减少了β-淀粉样蛋白斑块的人,而这种更常见的阿尔茨海默氏症并不是由基因突变直接引起的。它继续在两个大型全球III期研究中被研究。
索兰珠单抗
Solanezumab是一种抗体,旨在"清洁 "血液和脑脊液中的β-淀粉样蛋白,从而防止斑块形成。据报道,在整个三年半的试验期间,参加试验的人都有好处,而后来参加试验的人则较少,因此仍有更多关于其效果的知识。
多纳尼玛布
多纳尼单抗似乎是另一种即将到来的治疗阿尔茨海默氏症的有希望的药物。礼来公司正在对其进行测试,该公司计划在一项大型研究中招募1500名参与者,以确认其小型研究的结果;之前的这项研究持续了76周,包括257名患者,并且根据报告显示,多纳尼单抗显著减缓了阿尔茨海默病的进展。
其他
萨拉卡替尼是一种实验性化合物,它作为一种叫做Fyn激酶的蛋白质的抑制剂,帮助形成β-淀粉样斑块。在小鼠身上进行的一项研究显示,萨拉卡替尼通过抑制Fyn激酶,有效地逆转了小鼠的记忆丧失。抑制Fyn激酶可以防止或推迟疾病的发展。
加利福尼亚州索尔克生物研究所的研究人员正在研究一种叫做鱼藤素的化学物质,并开发了一种叫做CMS121的鱼藤素版本,他们发现该版本对减缓脑细胞的损失很有效。在药品可以获得批准之前,还需要更多的研究。
关于Aduhelm's recent approval, Maria Carrillo, Chief Science Officer for the patient-advocacy group Alzheimer's Association in Chicago, USA, said in a statement for Nature:"我们充满希望,这是一个开端--无论是对于这种药物还是对于更好的阿尔茨海默氏症治疗。"
"我们真正的身份是我们的思想和我们的大脑。"--桑迪,前牙医和助理教授,阿尔茨海默病患者。
everyone.org ,我们坚信,科学能够推动人类进步,改善甚至拯救生命。阿尔茨海默病正在危害许多人的生活质量。我们鼓励致力于寻找(部分)解决方案的科学家们坚持不懈地努力,我们期待着正在研发中的治疗方法能在未来 3 年内获得批准,让全世界的阿尔茨海默病患者都能获得治疗。


![最新批准的治疗克罗恩病的Stelara 替代品 [2024]](https://zh.everyone.org/media/blog/cache/336x_0/magefan_blog/julien-tromeur-7mnp_gV8TUA-unsplash.jpg)
![前列腺癌淋巴和骨转移的最新治疗方法 [2024]](https://zh.everyone.org/media/blog/cache/336x_0/magefan_blog/national-cancer-institute-SP2C8o2EZBw-unsplash.jpg)